Reducing infant and child mortality: assessing the social inclusiveness of child health care policies and programmes in three states of India | BMC Public Health

One way to assess a country’s economic performance is by looking at its mortality indicators because they not only manifest the economic disparities but also provide important insights into the nature of social inequalities [1]. The mortality rates of India have improved considerably during the last three decades—the infant and child mortality rates decreased from 86 and 119 per thousand respectively in 1992–93 to 41 and 50 per thousand respectively in 2015–16. However, the reduction in mortality was not commensurate with the high economic growth achieved since the mid-nineties [2, 3]. Besides, the progress made on the health front has not been uniform across population segments [1]. Our findings corroborate the later study, suggesting that the health inequalities, particularly the caste and tribe differences in child mortality have exacerbated in India during the post liberalisation era i.e., from 1991–92 to 2005–06.
In India, caste and tribe are markers for socio-economic status [4,5,6,7] and their association with infant and child mortality is well-established [1, 8,9,10]. Note, India, and especially rural India is considered to be one of the most rigidly hierarchical societies in the world. Here, different types of social stratification sort people into groups based on factors such as caste, religion or indigenous status. The caste system bestowed many privileges on those who are at the top of the caste hierarchy and imposed many social disadvantages including sanctioning of repression by the upper castes on those at the bottom. At the lowest rung of the caste ranking were the outcastes or untouchables. They are the present-day Dalits or Scheduled Castes (SC). Next in the hierarchy are ‘other backward classes’ (OBC), a collection of castes, which are not the victims of untouchability but they are still socially marginalised. The top-ranked castes are known as ‘upper’, ‘forward’ or ‘general’ castes. Scheduled Tribes (ST) are the Adivasis, who were subjected to severe forms of deprivation, and discrimination for centuries. According to Census 2011 [11], SC constituted about 16.6 percent of the Indian population, and a large percentage of them live in rural areas and are mainly landless agricultural labourers. ST comprised about 8.6%, while OBCs and general castes together accounted for 71 percent of India’s total population.
The recent round of data from the National Family Health Survey (NFHS)-5 (2019–21) [12] clearly shows the caste differentials in relation to child health status. The survey documents reduced access to maternal and child health services among the SCs and STs compared to the advanced castes. A decade before, the NFHS-3 (2005–06) [13] demonstrated a similar picture of poorer access and health outcomes amongst the disadvantaged social groups, which resulted in India not being able to achieve the health-related Millennium Development Goals (MDG) presented in Fig. 1.
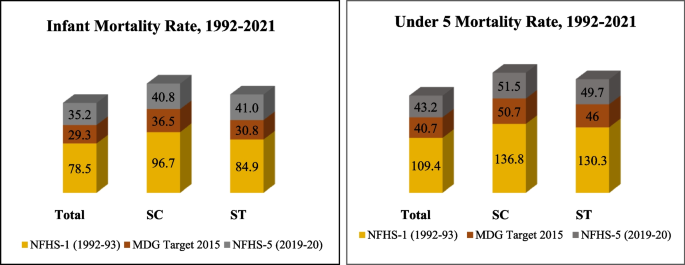
Achievements in reducing IMR and U5MR in India, 1992–2021
The term ‘social inclusiveness’ in the context of policies and programmes mean designing initiatives or undertaking policy reforms in ways which would ensure that the benefits of welfare programmes reach the socially marginalised populations. It has long been recognised that socially excluded population groups face not just economic barriers but also social and cultural barriers to access health services, yet the programmes are designed and implemented disregarding the above context.
Overview of India’s health care system reform and policy initiatives with special reference to child health care policies and programmes
India’s health sector has experienced major policy shifts since independence. Along with the overall changes in policy vision and goals, child health care policies and programmes have also evolved over time. From first five-year plan (1951–56) onward, a conscious effort was made to invest in health. In the early years of independence, the focus of health policies was mainly to develop national health programmes to control communicable diseases such as TB and Malaria, provide basic medical care, maternal and child health services (MCH) and family planning services.
Since the beginning of the plan era in 1951, population control has received disproportionate attention from the policy makers. In 1952, India became the first country in the world to launch a national programme for family planning. Health of the newborns and infants constituted a small component of this programme. After two decades, Govt. of India, in 1974, framed a national policy for children to prioritize child health, nutrition for infants and children in the pre-school age along with nutrition for nursing and expectant mothers while formulating programmes across all sectors [14]. Nevertheless, till 1977, family planning was the predominant health activity; As India’s vertical programmes like National Malaria Eradication and Family Planning Programmes achieved limited success, there were demands to critically evaluate them, which led to the incorporation of these programmes into the general district health services. Further, FP was modified into family welfare programme with MCH becoming an integral part of this programme with the understanding that reduction in infant and child mortality has a direct bearing on fertility (Govt. of India 2010). The diarrhoeal disease control programme was introduced in 1978 to prevent premature deaths of Under-5 children due to dehydration caused by diarrhea. In the same year, the Expanded Programme on Immunisation (EPI) was initiated to reduce morbidity and mortality from six vaccine preventable diseases, namely Diptheria, Pertusis, Tetanus, Polio and Childhood TB.
The vision of first National Health Policy (NHP), 1983 was to reduce IMR, NMR and CMR by the year 2000. In order to improve child survival rates, the government stressed on child health care programmes and particularly on childhood vaccination. The Government of India introduced Universal Immunisation Programme (UIP) in 1985 to remedy the shortcomings of EPI, The UIP was implemented in the country in a phased manner and was extended to the whole of India by the year 1990. Recognising the holes in the health care programmes for failing to adequately address high maternal mortality, a Child Survival and Safe Motherhood Programme (CSSMP), was launched by the Govt. of India. CSSMP subsumed UIP and it was implemented from 1992–93 to 1997–98 to improve the overall health of the infants, child and maternal morbidity and mortality. Besides improving the coverage of immunization services, CSSMP focused on interventions such as the Oral Rehydration Therapy, programme for control of Acute Respiratory Infection (ARI) in children, training of traditional birth attendants and strengthening of first referral units for providing emergency obstetric care to pregnant women. In order to address the unmet need for family welfare services in the country, especially among the poor and under-served, Govt. of India launched the Reproductive and Child Health (RCH) Programme for implementation in 1997 during the 9th FYP period by integrating CSSMP with other reproductive and child health services. RCH adopted Integrated Management of Neonatal and Childhood Illnesses (INMNCI). INMNCI case management strategy was designed to provide high-quality treatment for major childhood diseases in resource-poor settings. Aside from clinical management of these common diseases of the children, INMNCI also encompasses interventions to prevent them.
However, it is argued that the pressures from various quarters, particularly the international aid agencies which held the neo-Malthusian views on population compelled Govt. of India to make greater budgetary allocations for programmes directly or indirectly linked to population control, leading to crowding out of financial and infrastructural resources for other health programmes [15, 16]. Techno-centric approaches such as RCH were thought to be the key intervention to fertility decline. Consequently, the already limited public health care services such as MCH care, nutritional services and communicable disease control programmes, which had the potential to reduce child mortality and morbidity and thus, contribute to fertility reduction, became marginalised to make way for the expansion of RCH services. The RCH approach has also been questioned on the grounds that it did not recognise the linkages of reproductive health, general health and socioeconomic conditions [16, 17].
Numerous studies pointed out the inadequacies of the existing child health care programmes in terms of their limited scope and for not being able to ensure access of the vulnerable population groups [4]. For example, during 1980s, immunization rate among the most poor and marginalised children who needed the vaccines most was found to be the lowest [18]. The non-availability and low-quality health care for a prolonged period were largely responsible for high mortality and unmeasurable adverse health outcomes among the vulnerable population groups [19]. According to an estimate, India lost nearly 1.5 million children aged under-5 years annually [20]. To reduce inequity in health care services, Govt. of India launched National Rural Health Mission (NRHM) [21] in 2005 and National Urban Health Mission in 2008. These were later integrated under the umbrella of National Health Mission to strengthen the public health care delivery system in the country. Although NHM has a wide scope, its prime focus was on enhancing utilisation of Reproductive, Maternal, Newborn, Child Health and Adolescent (RMNCH + A) services among poorer and disadvantaged castes and tribes for reducing the maternal and child mortality [22]. Currently, under NHM, several schemes are being implemented to improve the health of the children.
In spite of these ongoing efforts and progress achieved, recent evidence suggests that access to maternal and child health care continues to be determined by socioeconomic status. For example, children, more specifically children of mothers experiencing deprivations in dimensions such as education, wealth and caste or tribe remained least likely to be fully immunized (Mishra and Shyamala 2020). It is worth noting that since independence India’s health policies and five-year plans [23] have recognised ‘caste’ as the source of poor health outcomes. The Bhore committee, in 1946 [24], in its report stated the following: “the poor state of India’s health, especially a section of people who were worse than the others in terms of health outcomes”. The NHP 1983 envisioned to achieve ‘Health for all’ by rolling out a universal comprehensive primary health care services programme, which would effectively address the perennial issue of exclusion of the most marginalised populations from the benefits of public health services by the year 2000. In a similar vein, the 12th five-year plan document states that “barriers to access would be recognized and overcome especially for the disadvantaged and those living far from facilities”. However, despite the governments committing to making health care accessible to everyone, adequate efforts were not made to translate this goal into action. To put it in perspective, the public investment in health did not exceed beyond 1% of GDP even during the high growth years in 1990s. Barring a few changes at the programme level, there was hardly any major health sector initiative during the 90 s. The first decade of the twenty-first century was little better. The launch of NRHM is considered to be a watershed moment for the health sector, though the budgetary allocation has been inadequate [25].
Health inequality is a topic of longstanding interest in India. Historically, the health policies and programmes have tended not only to improve overall population health but also to reduce differences in health based on region/state, caste/tribe, socioeconomic status and other social determinants. This article seeks to produce evidence to assess the contributions of the above-mentioned policies to the realization of the health equity goal, specifically the caste/tribe differentials in infant and child mortality.
Review of past studies
There is a growing body of literature, which sought to understand the social group disparities in health and health care in India. Studies observed that health outcomes among SCs and STs are strongly linked with their overall deprivations emanating from the social and economic relations of the caste system, which are created and reproduced in all spheres of life. Remoteness, poor diet, underdevelopment, illiteracy, and limited access to healthcare continue to have robust bearings on marginalized communities’ health outcomes [8, 26,27,28]. A study by Ranjan et al. [29] concluded that the gap in infant mortality between tribal and non-tribal populations was substantial in the early months after birth, narrowed between the fourth and eighth months, and grew thereafter. Another study by Dommaraju and colleagues [30] demonstrated that children born to ‘lower’ caste families have a relatively higher risk of death and that women belonging to the lower castes have lower rates of antenatal and delivery care utilization than children and women from the upper caste families. In light of this evidence, the researchers of the above study argued for embedding pro-disadvantaged caste and tribe bias into the provisioning of maternal and child health services. Baru and colleagues illustrated that aside from facing socioeconomic backwardness, people from disadvantaged castes experience other adverse circumstances such as caste-based discrimination while accessing the health service system in India [1]. Studies also illustrate that disadvantaged castes and tribes still have unacceptably high child and adult mortality and persistently lower life expectancies than advanced castes [31, 32]. Further, SC and ST mothers accounted for almost 50 percent of all maternal deaths in the country, and their children were more undernourished compared to the rest of the population [33, 34].
The current study builds on the existing literature on caste and tribe differences in infant and child mortality. The point to be noted is that despite the flagship maternal and child health (MCH) programmes, the caste and tribe disparities in child health are still persisting. Existing studies sought to identify the determinants of infant and child mortality among social groups by focusing on the national level and not on the state level. Besides, there were limited attempts to examine the factors that affect the survival status of infants and children among depressed castes and tribes in India. As discussed earlier, there were some significant health policy developments in the past one and a half decade to improve maternal and child healthcare. The effects of these initiatives on improving the state of child health for the marginalised communities have remained mostly unexplored, and that make this research more relevant. Hence, this paper’s first main contribution lies in the fact that it disaggregates childhood mortality into infant and under-five mortality and analyses the correlates of each using the latest round of NFHS (2019–21) data. The second main contribution of this paper is that it provides evidence on the effect of caste and tribe on infant and U5 mortality in three different states. Our study’s findings can help to understand the factors behind the persistent gap in IMR and CMR between deprived castes and tribes and advanced caste groups in those three states of India.
link





