Questioning global health in the times of COVID-19: Re-imagining primary health care through the lens of politics of knowledge

The idea of PHC acquired prominence through the innovative Alma Ata documents of 1978 that championed the call of ‘Health for All (HFA) by 2000 AD’ through a PHC approach. Foregrounding the four principles of equity, community participation, appropriate technology and inter-sectoral coordination, PHC was proposed as an instrument to “close the gap between the haves and have-nots, achieve more equitable distribution of health resources, and attain a level of health for all the citizens of the world that will permit them to lead a socially and economically productive life” (WHO-UNICEF, 1978). Despite its limitations as a negotiated document across the geo-political divides of that time, it was successful in legitimising two central ideas—one, health is mediated by factors beyond those that are medical in nature, and therefore, development in other sectors as well as inter-sectoral coordination is essential for HFA; and two, the desirability of quality health services and health workers close to the community and community’s participation in taking care of its own health. Thereby it implicitly shifted the exclusive locus of health knowledge away from the doctor and hospital to paramedics, community health workers and communities (Priya et al., 2019).
Re-reading history: a gap analysis
The causes for the limited adoption of the PHC approach have been located largely in the political economy of the medical establishment, the international economic order or in national governance flaws (Navarro, 1984; Phadke and Shukla, 2006; Labonté et al., 2017). Also, community participation, adoption of appropriate technology and inter-sectoral engagement were found to be the weakest strands in PHC implementation (Lawn et al., 2008). Lately, there is a demand for recognising “community health systems” and acknowledging various resources and skills available in community settings that can be utilised in the healing process (Emerson and Nabatchi, 2015).
In an attempt to complement these analyses with insights obtained using the PoK lens, we seek to understand the knowledge that has been instrumental in guiding the framing of the Alma Ata documents that articulated the PHC approach. Further, this paper attempts to develop the dimensions of PoK that will be able to effectively shape the health systems in the spirit of PHC (Priya et al., 2019).
The spirit of the Alma-Ata document (WHO-UNICEF, 1978) includes social justice, people’s empowerment, and economic sustainability. With health visualised as an individual and collective attribute and an outcome of societal conditions, the document framed health services from the perspective of overall development. Emphasis was placed on contextually relevant healthcare, appropriate technologies and healthcare providers at levels as close as possible to the users. This led to the development of primary-level health services including community outreach across the world. Further, this ensured provisioning of mass healthcare by extending the legitimacy of health knowledge holders and practitioners from doctors and hospitals to paramedics and communities. However, its impact on health services was limited due to the political economy of the medical-industrial complex that continued to dominate. We argue that this was allowed by the Alma Ata report due to its lack of explicit acknowledgement of the PoK and addressing of its inequitous consequences in operational terms. This contributed to the subsequent limitations in knowledge translation and continuing legitimacy of the path to techno-managerial care.
It should be recognised that the Alma-Ata report (WHO-UNICEF, 1978) was neither adequately explicit about the inherent value of ‘people’s knowledge and perceptions’, nor about ‘people’s empowerment’, despite its emphasis on ‘community participation’ and health services being ‘acceptable to the people’. Its articulation maintained an uncritical epistemic supremacy of conventional expert-led biomedicine. It accepted the hegemonic position of ‘modern’ medical science and technology which require people to be educated to use them appropriately. This led to PHC strategies designed to attain ‘health for the people’ and ‘health with the people’, but rarely ‘health by the people’. This neglect resulted from biomedicine being considered as the sole legitimate health-related knowledge and therefore, medical professionals as the natural knowledge leaders of the health system (Priya, 2022). Further, presenting PHC as a vision for the first level of care rather than for the whole health system led to it being largely perceived as addressing the lowest, i.e. the primary institutional level without affecting the structure and content of secondary and tertiary hospital services.
There were other inconsistencies observed in the document too. Though the focus of the document rested on primary-level care, it was still considered located at “the periphery”, while secondary and tertiary levels remained “the centre” of health services (Ghodajkar et al., 2019), as in Fig. 1. Doctors and hospitals remained the bearers of supreme knowledge that had to be taken to the periphery through ‘outreach’ services. ‘Iatrogenesis’ [i.e. the ill-health generated as a result of medical interventions (Illich, 1977)] and the ‘unaffordability’ of services due to the proliferation of the medical industry and private sector went unaddressed; professional ethics was not mentioned; the environmental consequences of development which had not yet crystallised in public discourse by the 1970s were missing.
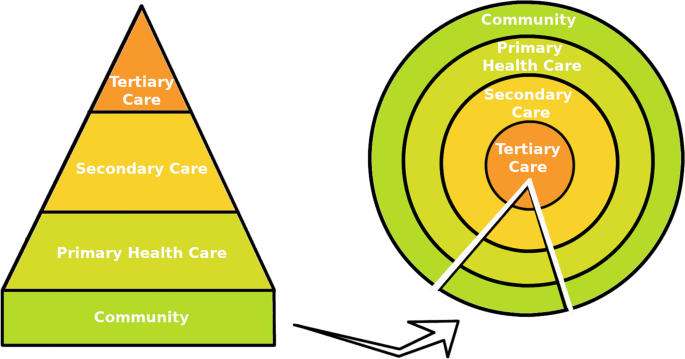
Source: Modified from the authors’ initial work; Ghodajkar et al. (2019).
While the centrality of the community is underlined as a value in the Alma Ata declaration, calling it peripheral is an internal contradiction. However, this contradiction is in consonance with the exclusion of laypeople’s health-related knowledge and practices in operational designs. Also, it led to a lack of in-depth attention to ‘the community level’ and its complexities as well as the operational requirements to strengthen health actions within it (World Health Organization, 2009; Savatagi et al., 2022). The ‘community’ was perceived as a homogenous entity, overlooking the hierarchies and contestations within it (such as class, race, caste, and gender). These contradictions of the Alma Ata document sowed seeds contributing to its limited implementation, further compounded by the antipathy to CPHC and democratisation of PoK of the medical–industrial complex and its professional, political, technocratic, and commercial interests.
The negotiated drafting of the Alma Ata documents had resulted in the omission of the politics of governance and critiques of the dominant biomedical knowledge and its practice. These gaps allowed the misinterpretation of the spirit of PHC as a mere techno-managerial systems design devoid of its dimensions of power. This allowed Selective PHC with an ‘essential basic healthcare package’ to be argued for as a feasible approach for implementing PHC (Walsh and Warren, 1979) over the more complex social, political, and cultural task of Comprehensive PHC. It initially got reduced to GOBI-FFFFootnote 2 which attempted to bring biomedical understanding to benefit vulnerable women and children through globally orchestrated mass ‘campaigns’ for non-medical and medical interventions (Chen, 1988; Wisner, 1988). Hence, the requirement to understand people’s context, local resources, self-reliance and wider determinants of ill-health was eliminated from the PHC approach. The next advancement was the propagation of the new epidemiological tool of DALYs-based cost-effectiveness analyses that posited prioritisation of public health agendas based on decontextualised global epidemiological datasets and demonstrated the advantage of medical technological interventions over upstream non-medical interventions while claiming the application of the principle of ‘equity’ (World Bank, 1993; Priya, 2001; Barker and Green, 1996; Rao, 2009). This further skewed the system against local priorities and community-led initiatives (Banerji and Andersen, 1963; Banerji, 1995; Peralta, 2018). Empowerment, thus, was presented by the knowledge generators and translators of the dominant public health system as the ability to “consume” global expert-defined “entitlements”, rather than gain actual control over their own health and its determinants. The ‘selective’ translation of PHC suited the technocratic health bureaucracies, the political leadership and health professionals as it did not demand any significant shifts in power equations even when it led to engagement with the underserved communities. These were the communities who were considered reticent in utilising ‘modern medicine’ and contraception, or a more empathetic understanding was that they were the ‘unreached’ and therefore, GOBI-FFF was to be implemented in a top-down orchestrated ‘campaign mode’ (Chen, 1988). The larger shifts in approach to health care required for translation of Comprehensive PHC into policy and practice—the need for bottom-up knowledge and its application, health technology assessment for ‘appropriateness’, and changes in secondary and tertiary level services as supportive of the PHC approach—were side-lined. Traditional healers were referred to as community influencers to be utilised for primary-level conventional biomedical services with appropriate training, rather than as holders of useful knowledge:
“Traditional medical practitioners and birth attendants ….are often part of the local community, culture and traditions and continue to have a high social standing in many places, exerting considerable influence on local health practices. With the support of the formal health system, these indigenous practitioners can become important allies in organising efforts to improve the health of the community … It is, therefore, worthwhile exploring the possibilities of engaging them in Primary Health Care and of training them accordingly.” (WHO-UNICEF, 1978, p. 33; emphasis added).
It provided a tenuous thread to a third strand that attempted to use the PHC discourse to promote medical pluralism in health systems development (Payyappallimana, 2010; Shankar, 1985). Thus, there was the dominant operational policy translation of the concept of PHC to Selective PHC, a significant conceptual acceptance but marginal operational translation of Comprehensive PHC, and an even more marginal translation to a system of Comprehensive PHC with a plurality of knowledge (Priya, 2018).
The post-2000s period saw the rise of the idea of UHC which with several iterations has come to be restricted to ‘ensuring medical care to all without financial catastrophe’ via expansion of medical insurance coverage (WHO, 2009; Baru, 2012; Sanders et al., 2019). The question, ‘why medical expenditures were becoming increasingly unaffordable despite cost-effectiveness exercises’ was never asked. From Alma-Ata to UHC, physical iatrogenesis along with social and cultural iatrogenesis (Illich, 1977), remained unacknowledged. On the other side, the state and private commercial interests of the medical–industrial complex came together to shape knowledge as they wanted: to ‘serve’ the population as passive consumers.
However, despite this onslaught, people’s own wisdom prevailed and non-dominant forms of knowledge continued to be in practise. For instance, while the national and global governance responses to COVID-19 involved primarily top-down command and control measures or market approaches with individualised risk-management advisories to ‘stay home and keep your family safe’, the world witnessed an unprecedented level of community action of solidarity and support too. People’s responses ranged from personal preventive measures using home remedies and traditional medicine to a wide variety of community-driven efforts such as awareness campaigns, tele-consultations, and social support measures (Lowensen et al., 2020; Priya et al., 2022).
While this persistence is either ignored or seen as an aberration, we argue that it is more productive to view this persistence as a means of filling the gaps of dominant healthcare, and as resistance to its multi-faceted iatrogenesis.
Traditional health knowledge systems: a case in point
Historically, all societies and communities have developed modes of health care (promotive, preventive, curative, palliative) followed by the state emerging as a major provider to the masses in the last two centuries. While this has increased access to conventional (‘modern’) medicine tremendously, it has induced delegitimisation and displacement of the prevailing popular knowledge and practices in parallel.
The value of traditional knowledge, both folk and codified, lies in them being closely related to ecological worldviews (Payyappallimana, 2010). Required material resources are available in natural surroundings and have been traditionally accessible to all including the poorest sections whose livelihoods and life patterns bring them in close contact with nature. These systems are close to popular cultures that people identify with and are also considered to be safer and sustainable (WHO, 2002). They have also made significant contributions to the development of pharmacology and pharmacopoeia of ‘modern’ biomedicine (Rubira, 2011). Their ‘whole systems approach’ rather than the analytical reductionist approach of conventional biomedicine provides an epistemic holism that ‘systems biology’ and its medical applications are just beginning to explore (Payyappallimana et al., 2020).
This epistemic diversity has been asserted since the colonial era of the 19th and 20th centuries in India and elsewhere (Hunt, 1999; Sivaramakrishnan, 2006; Sharma, 2013; Bala, 2014). The contingencies involved in making healthcare accessible to large masses of Asian countries such as China, and during the course of the HIV epidemic in Africa brought in official support in the second half of the 20th century leading to WHO’s policies on traditional medicine (WHO, 2002, 2014). The ongoing relevance of these knowledge systems is reflected in the resurgence of ‘bio-prospecting’ by pharmaceutical companies (Mgbeoji, 2006). Yet, neither in PHC 1978 nor in UHC 2018 does global health discourse give this epistemic pluralism any space and therefore, the two discourses of universally accessible health care and resurgence of traditional health knowledge systems run in parallel. The Astana declaration and its supportive documents demonstrate some move towards recognising the value of traditional knowledge, but there is little by way of operationalising its use (Priya, 2022). The challenges faced by various national health systems during the COVID-19 pandemic also displayed similar disjunctions, making a vast repository of knowledge base, human and institutional resources redundant in the official response (Sujatha, 2021).
COVID-19 management as anti-thesis of the PHC approach
The management strategies of the COVID-19 pandemic illustrated the antithesis of the PHC approach in the choice of knowledge adopted for policy and its translation into techno-managerial measures designed for the prevention of cases as well as care for those manifesting symptoms. These manifestations in the backdrop of the Astana Declaration of 2018 (which espouses UHC-with-PHC) demonstrate the consequences of Selective PHC and of the subsequent global health discourse that informed health systems development, denying the validity of multiple epistemologies, people’s knowledge and practices, bottom-up and context-sensitive plural solutions.
During the initial period of the COVID-19 catastrophe, pandemic management in India and across the world was largely dominated by a global narrative of lockdowns informed by modelling exercises conducted by global health institutions (Ferguson et al., 2020). The overall experience of pandemic management displayed an ahistorical, decontextualised and narrowly focused medicalised understanding that involved controlling the spread of the virus through lockdowns and provisioning of treatment through scale-up of ICUs and ventilators ignoring the wider social, economic and health impacts. Reliance on the development of a vaccine to contain the virus transmission and reduce serious cases and deaths prevailed, ignoring the role of natural immunity completely. A false dichotomy was often created between saving lives and saving livelihoods to legitimise the tradeoffs (Prasad et al., 2020). Questions that ought to have been asked were, “What works best, for whom, under what conditions, what are the unintended consequences and who pays the costs?” (Priya et al., 2020a). In addition to the immediate firefighting, long-term public health thinking about the pandemic and its impact was required. Instead of the command and control approach to public health witnessed in global and national responses to the pandemic, there were demands from many quarters for a comprehensive public health approach that would competently address different social needs and health requirements of different sections of people, with participatory decision making and action (IPHA, IAPSM, IEA, 2020; Loewenson et al., 2020; Priya et al., 2020a; Prasad et al., 2020; Priya and Dasgupta, 2020).
In the context of patient care of COVID-19 cases, strong PHC-led health systems, usually the first point of contact, could not only have addressed the essential healthcare needs of most of the uncomplicated cases but could also have played a significant role in arresting the spread of the pandemic through monitoring, detection and prevention of early signs of an outbreak (WHO, 2021). In fact, around 80% of the COVID-19 patients had only mild illness, about 15% required oxygen support and only 5% needed intensive care. A bottom-up PHC approach would have mobilised community-wide networks of frontline health workers and local volunteers to provide the much-needed psychosocial support and pertinent advice on home-care after the diagnosis of COVID-19 (through laboratory tests) minimising the unnecessary rush to hospitals by those testing positive but with mild symptoms (Kulldorff et al., 2020). Simultaneously, the suffering and deaths of moderate and serious cases would have been minimised by the latter’s monitoring of danger signs and linking of complicated patients with advanced facilities as required. Instead, the focus was on converting tertiary care centres into designated COVID hospitals, creating extra ICU beds and over-stretching hospital capacity, overburdening the health workforce and severely jeopardising treatment of other complicated illnesses. However, the primary-level workers were intensively utilised for the administration of the vaccines against COVID-19 after they became available.
The current form of knowledge governance with global health’s singular techno-managerial solutions was at play instead of a comprehensive, contextualised, people-centric public health reasoning. This hegemonic practice places simplistic epidemiological uni-causal germ theory thinking over the reality of complex multi-causal epidemiology and technological solutions on people. Therefore, the vaccine is presented as the panacea and lockdown as the only legitimate interim measure, countering any need for epidemiologically informed context-specific preventive efforts and/or provision of primary-level supportive care for those asymptomatic or mildly affected, and over-dependence on ICUs and ventilator support (Priya and George, 2022). In this hierarchical relationship, complementarity of solutions is not acceptable and the knowledge adopted for translation into action is mediated by the PoK, the unequal distribution of power among the global community of nations and the medical industrial complex; a greater legitimacy for the positivist disciplinary moorings of mathematical modelling and the uni-causal germ theory; and a denial of validity to diverse strategies and measures suited to heterogeneous economic, social and cultural contexts.
Against this backdrop, this gap analysis asserts that, if the PHC approach is to be effectively implemented, it must be reconfigured to address the PoK underlying the relationship between conventional biomedicine and other knowledge systems as well as between the communities’ cultural and experiential knowledge and that of the biomedical professionals. In the next section, we adopt a PoK lens to propose a health systems design for PHC 2.0 that could reorient the translation of the PHC approach into context-appropriate policy and practice.
link








